1. Joined a photographic society
One of the biggest differences of this year was joining The Societies of Wedding and Portrait photographers and I have been making great use of all their benefits. I have submitted to their monthly competitions and even won a highly commended award! I also won a highly commended award for two further images with the National Photographic Society (NPS). I also use their mentor program, which has been a game changer for me.
2. 1-1 Training
The training day I had with Gary Hill (The Art of the Portrait) made me completely revaluate all my previous work! I feel like I can see much more clearly what I need to improve on and how to achieve what I want to before a session. I can plan effectively with lighting and posing and can focus more on connection with subjects during a shoot. Below are two portraits I captured during the training session.
3. Upgraded to Strobe Lighting
One of the first steps to improving my photography this year was to upgrade my current lighting system from continuous to strobe lighting. I did a lot of research into this and decided to go with 'Elinchrome's D-Light RX 4's. They have been amazing and honestly have taken my photography to the next level.
4. Upgraded Backdrops
I also decided to switch from my vinyl backdrops (which are still great as wipe-clean options for cake-smash photoshoots) to fleece backdrops, from Kate Backdrop. I initially bought them as they were able to ship quickly and I wanted a more painterly look. They look so beautiful in the final images and so I have ordered more of them since! The texture is beautiful and they look very painterly. They are also much bigger backdrops, so I can fit many more full length people in family photoshoots than before, and still have room around the edges!
5. Lightroom to Photoshop
For the majority of my work, I have previously been using lightroom. I kept photoshop for making big changes to an image such as swapping faces or newborn composites. I am now moving my whole editing process over to photoshop as, although it is more time consuming, I truly believe I am able to offer a much more refined image through the extra tools on there. I am easily able to enlarge and reframe each image, rather than only being able to crop smaller. Textures, brushes and colour adjustment are also a lot more effective. I could spend a long time explaining more, but instead, I have shown the difference below - yes, they are the same image; I have used parts of other images in photoshop to make the family's pose flow better.
6. Won three awards!!
I felt very nervous to enter competitions this year for the first time! I was really encouraged by the process and that I actually won three highly commended awards this year (two below and one was at the top of this blog)!
7. Published!!
I was absolutely thrilled to have my work published in Child Couture Magazine in their December 'Wonderland' Issue.
8. Featured
I submitted some of my images to be featured for the first time this year. I was very proud for my images to be selected and featured by Gallery of Refined Art (on facebook) and Rise International Photography Awards (on instagram).
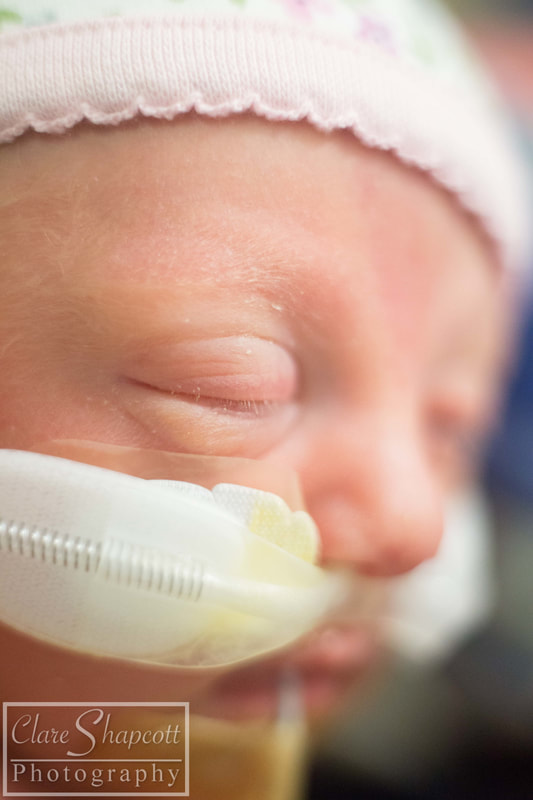
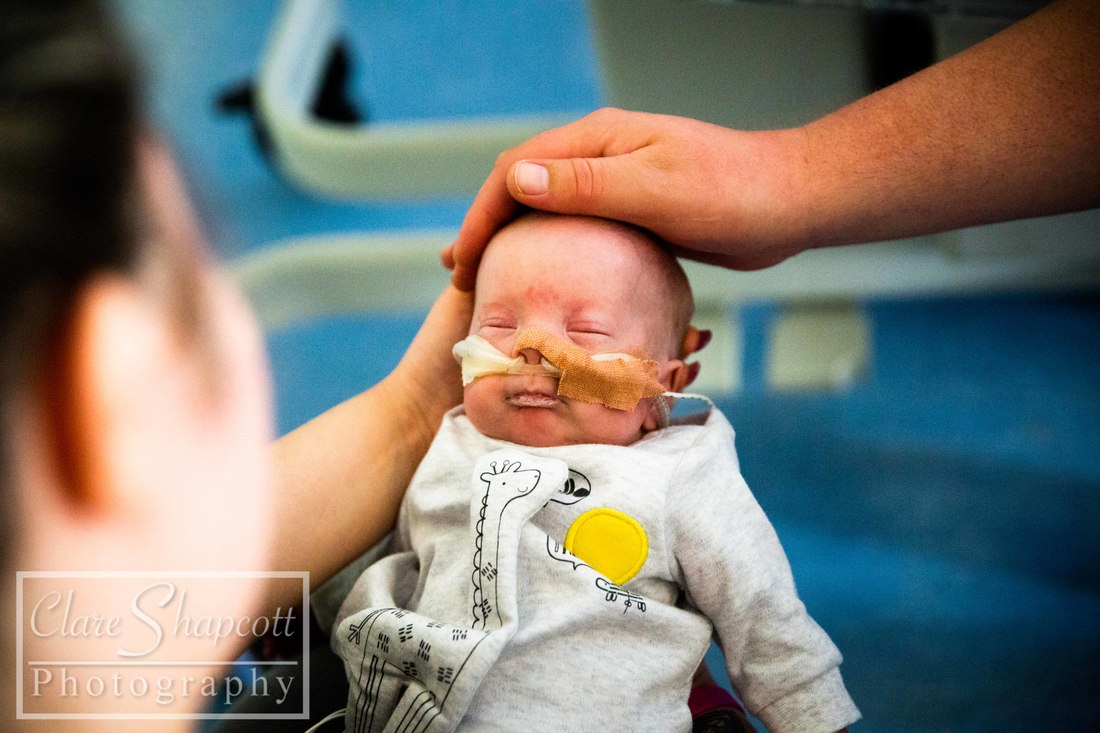
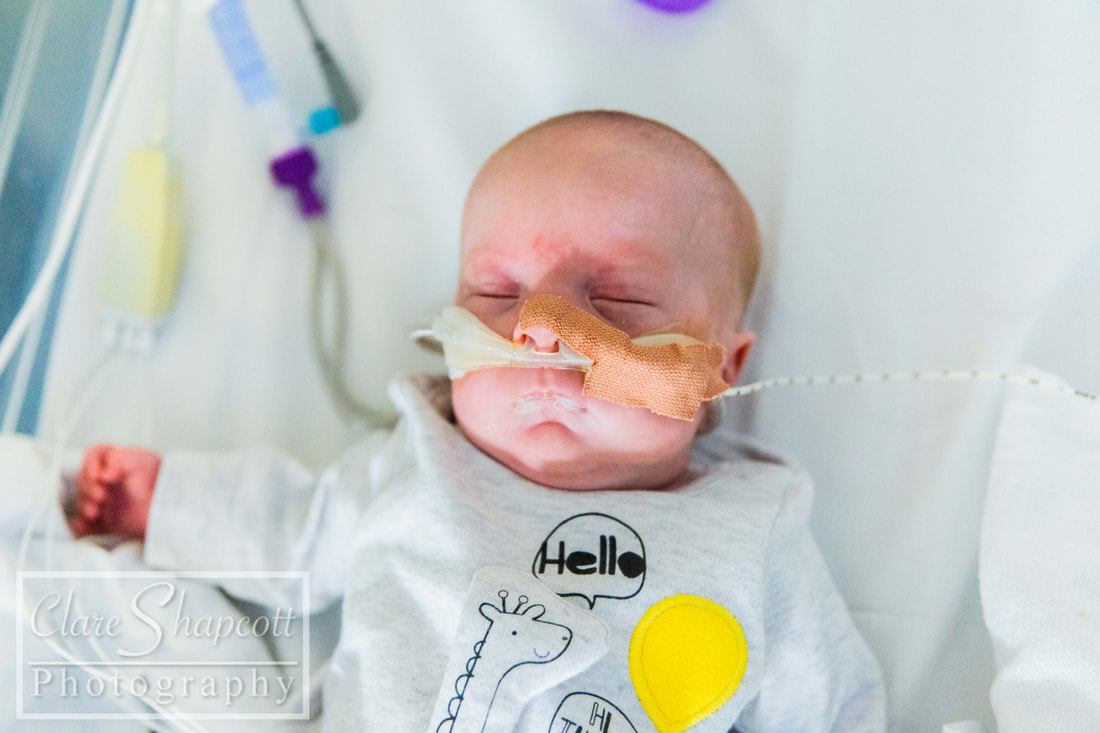
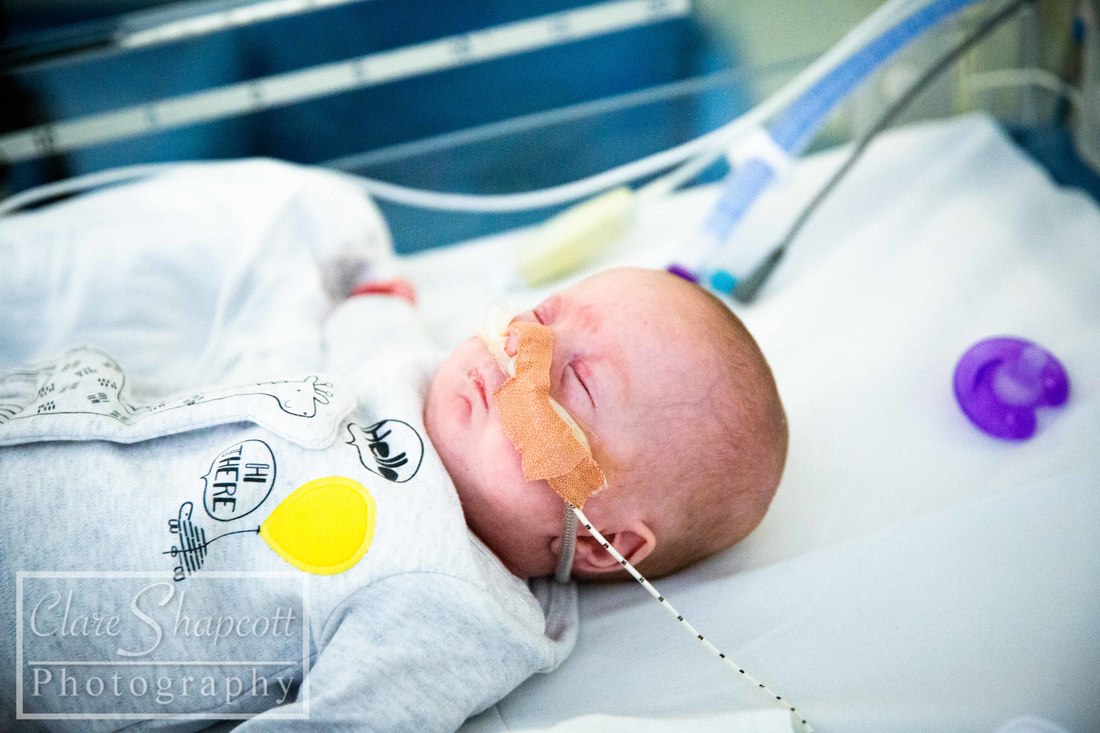
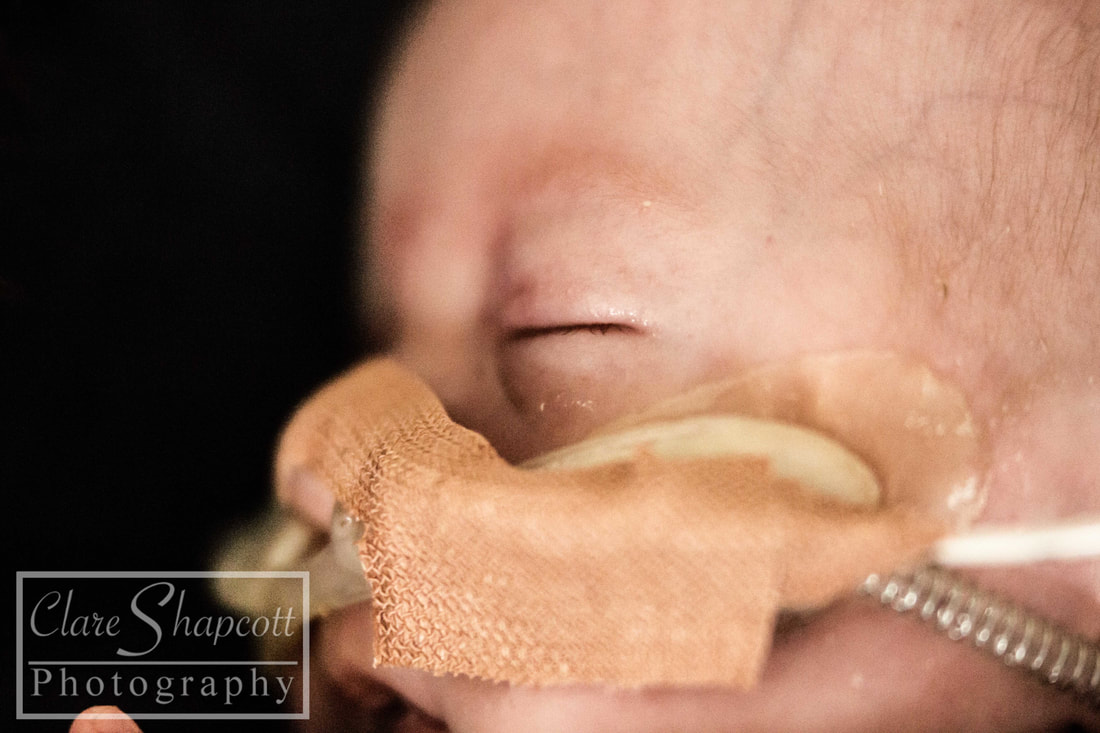
9. NICU Project
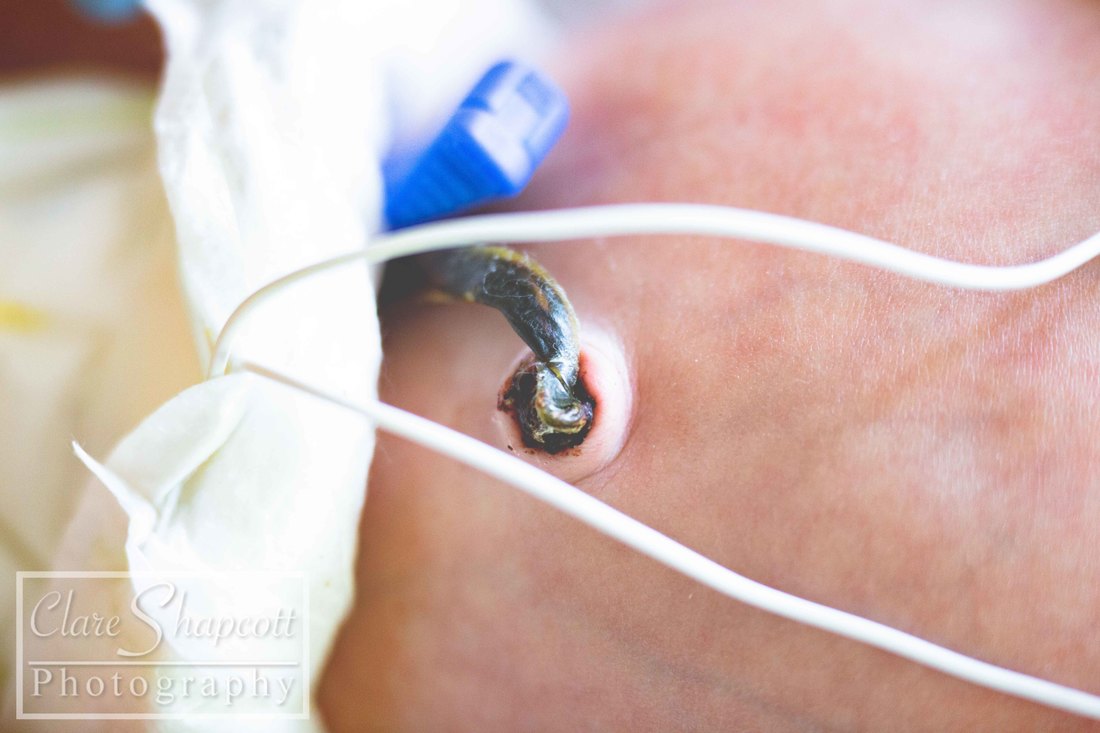
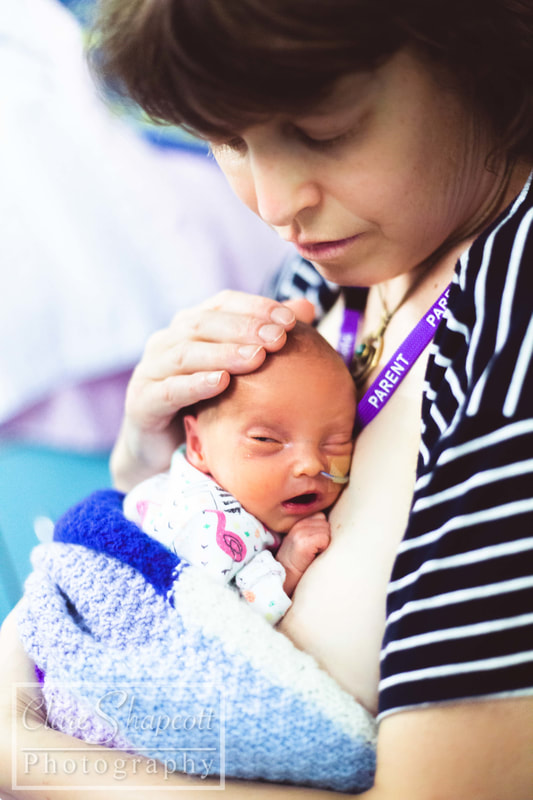
I am still offering completely free NICU photoshoot sessions to parents with babies at St Michael's and Southmead NICUs. I am planning to continue this as long as possible despite things becoming more busy in studio! I love this project as it has helped me make a difference to many parents in such a difficult situation and provided something 'normal' in a circumstance that is far from it! My work there was featured on BBC Radio Bristol (on facebook) and I was also interviewed on their breakfast show.
You can find the interview for BBC Radio Bristol's Breakfast show here:(2:07:00): https://www.bbc.co.uk/sounds/play/p07f0j4q Find out more about my voluntary NICU photoshoots here: N.i.c.u Sessions.
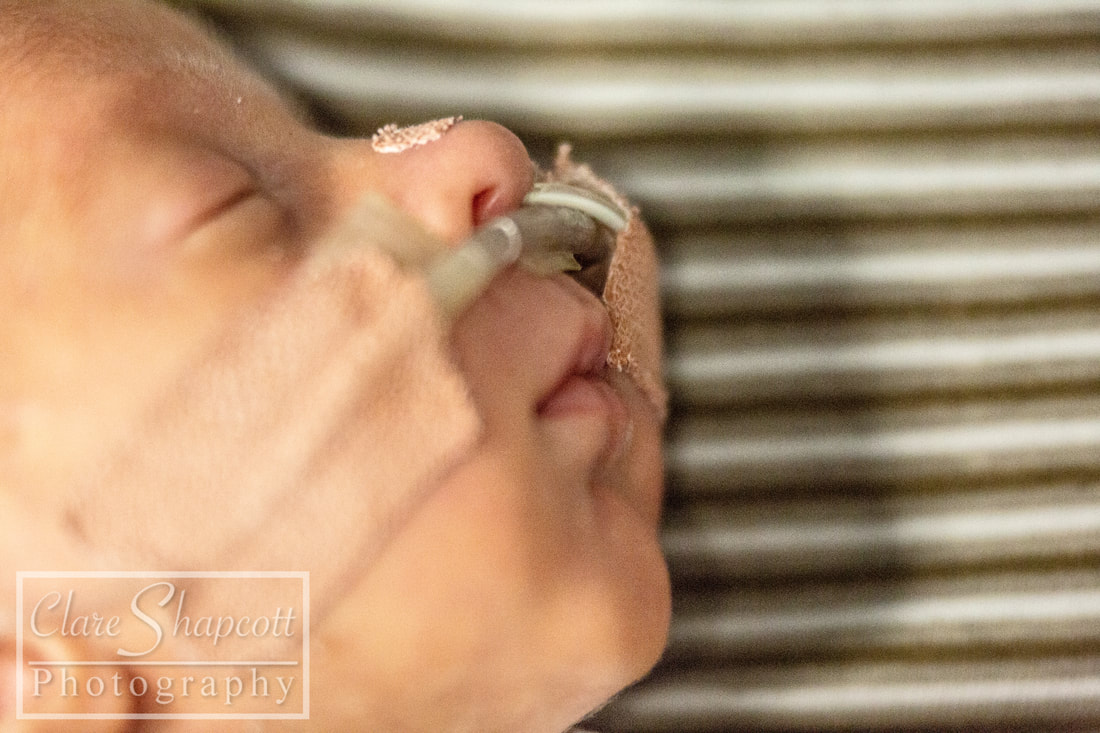
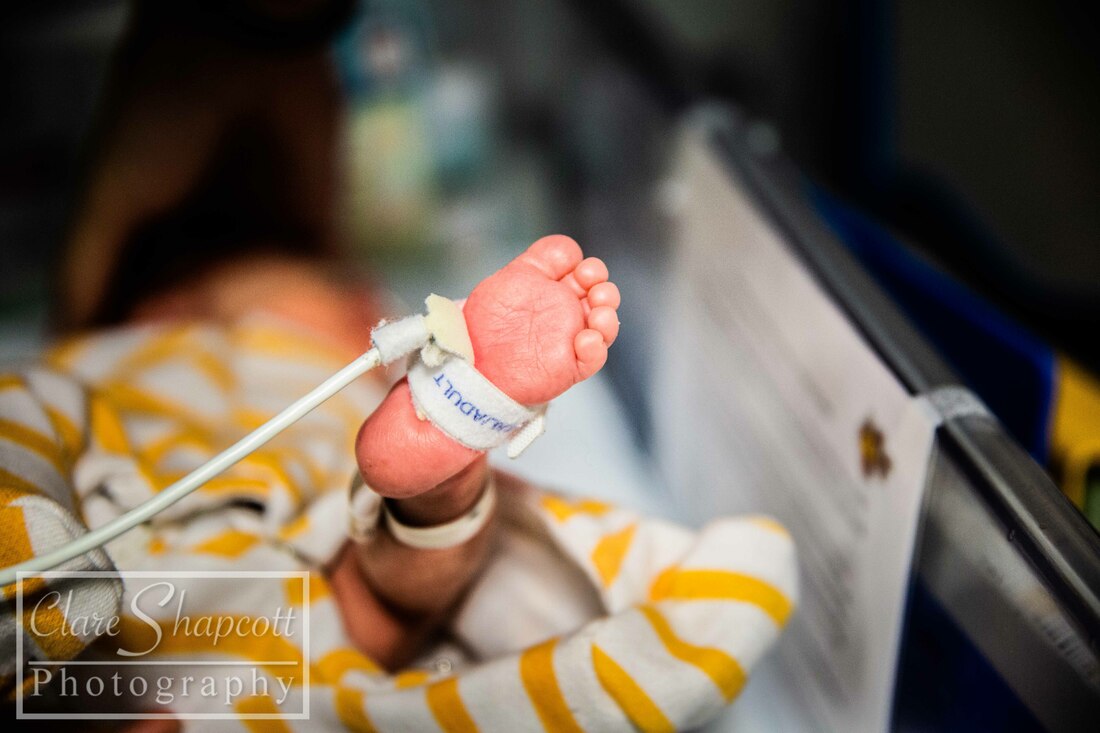
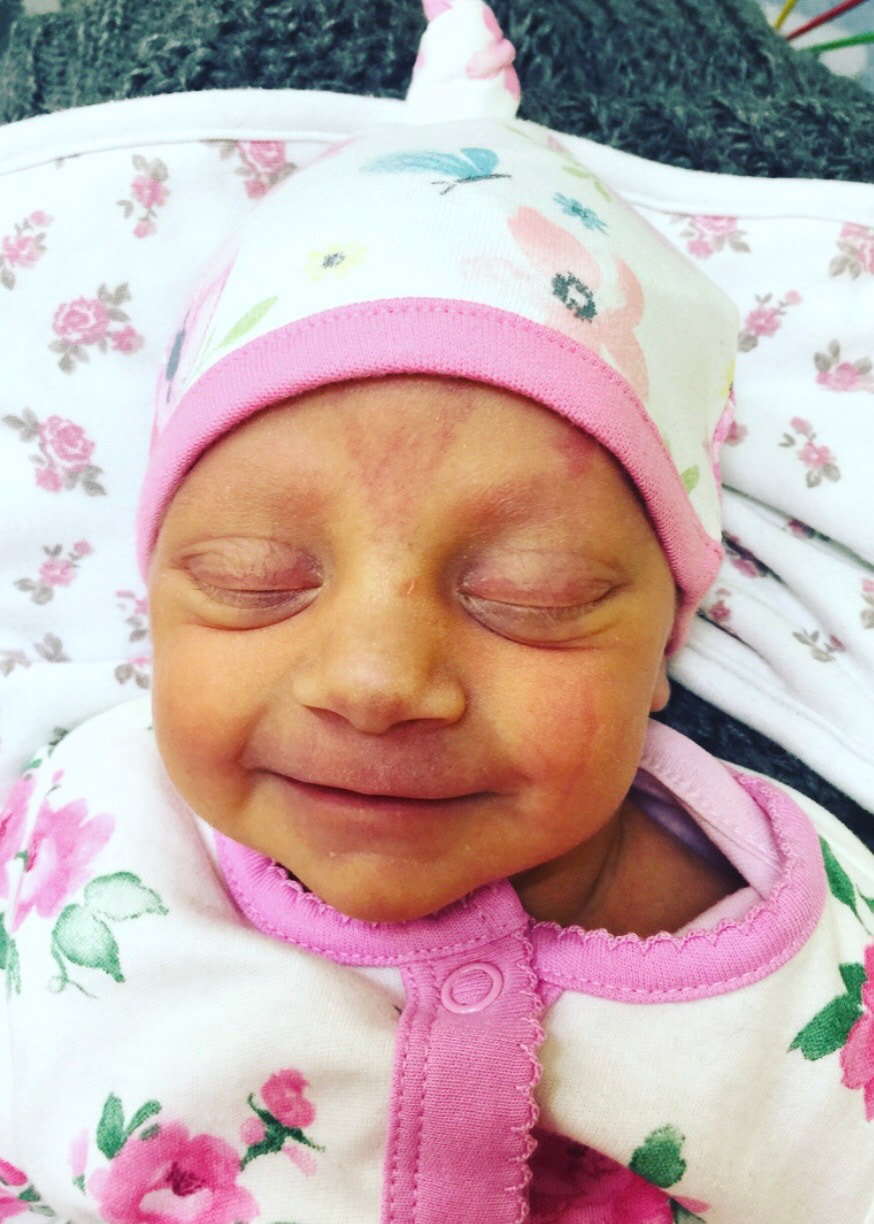
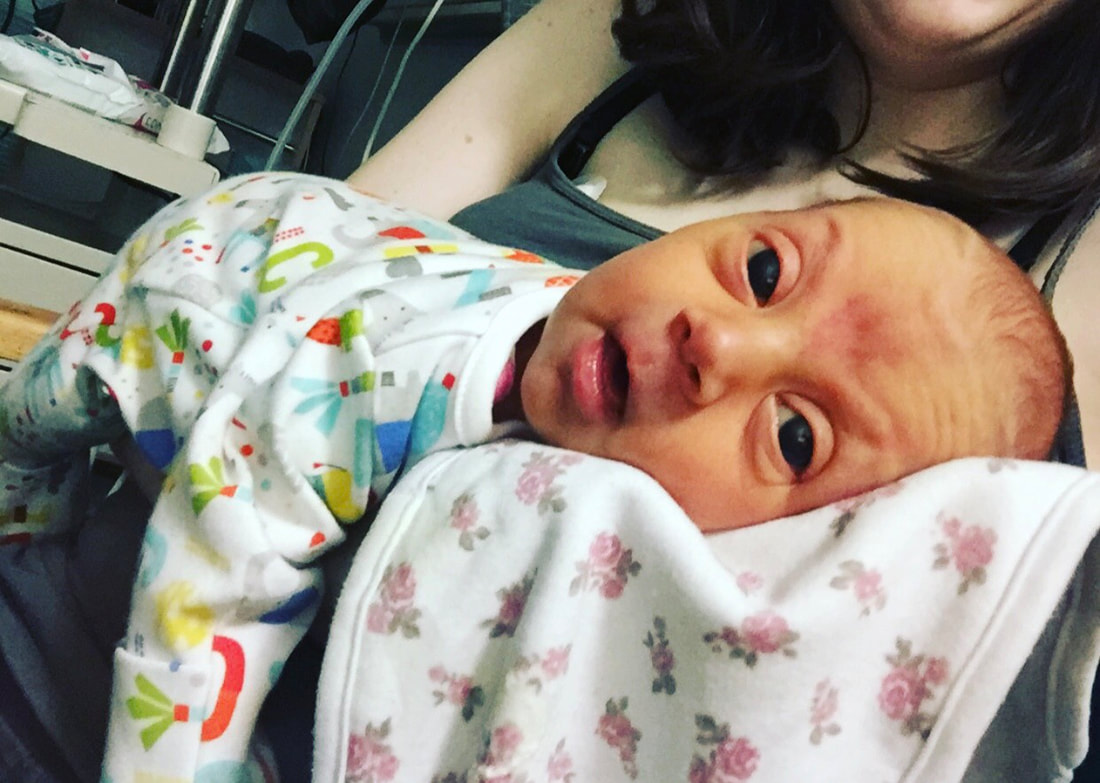
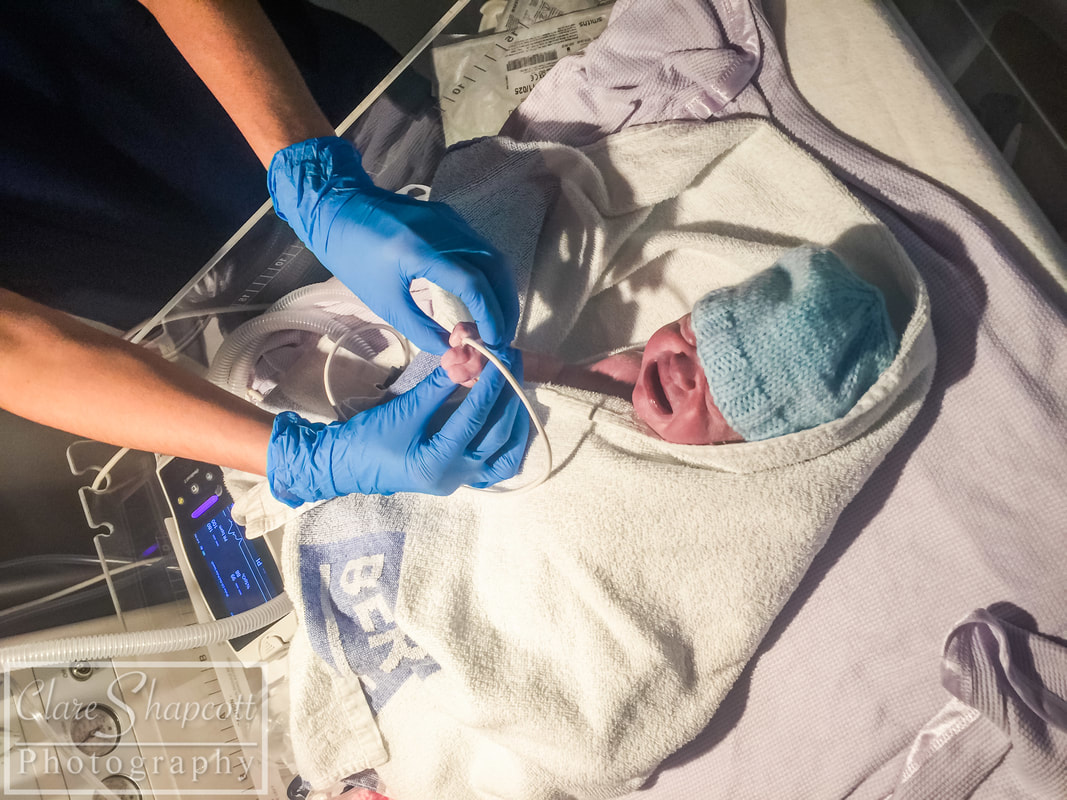
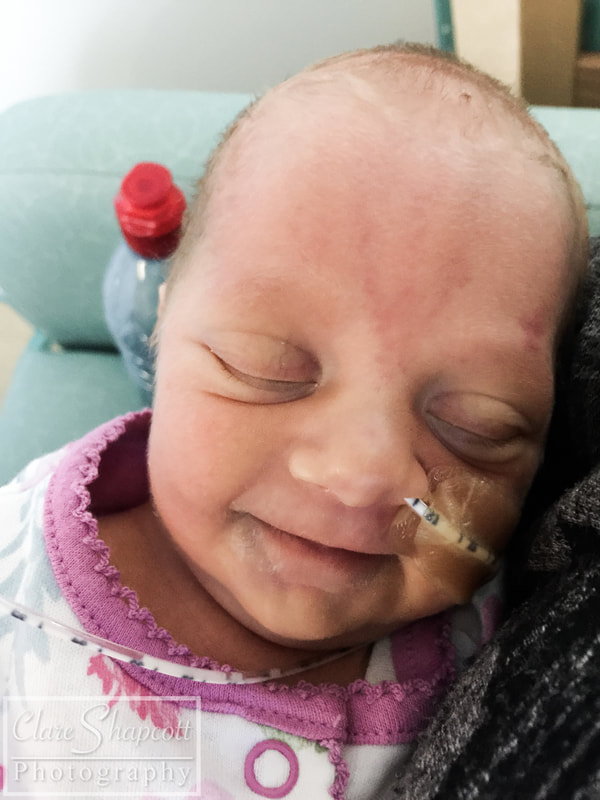
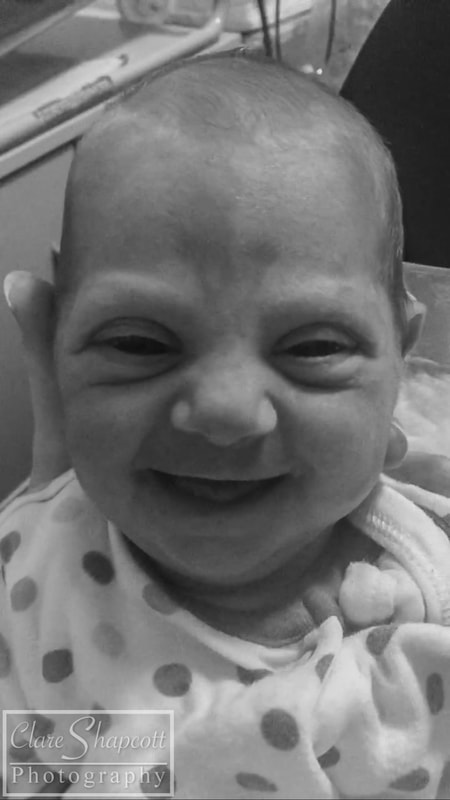
I met Cindy last winter at St. Michael’s hospital where she gave birth to her incredible son, Elliott, at 29 weeks gestation. Up until 28 weeks, Cindy had a textbook pregnancy. She felt nauseous during her first trimester, but apart from that she was doing well. She was attending pregnancy yoga classes, and had just returned from a holiday in Scotland where she had been hiking. At 28 weeks gestation, after a lovely day of music and dancing at St. Paul’s Carnival, Cindy’s waters broke, and she was told to go to St. Michaels hospital so that her baby could be monitored. She was there for five days, and everything appeared to be fine, so she was discharged and given antibiotics to prevent any possible infection due to the premature rupture of her membranes. She returned home, but was shortly met with a surprise! Her waters broke again after being home for only 6 hours. Cindy went back to St. Michaels Hospital and her baby was monitored once again. This time, however, Elliott had no intention of staying in his mum’s tummy, and, as Cindy had put it “he decided it was time to discover the world!”. Elliott was born at 29 weeks and only weighed 1.5kg (3lbs 5oz), yet he still managed to let out a huge cry. Elliott needed some extra help to breathe, so he started to use a CPAP machine (a machine that helps to inflate the lungs in-between breaths), before going onto a high flow and then a low flow cannula which helped air to flow into his lungs. Cindy says that her happiest moment was when she and Elliott had their first cuddle. Two nurses were required to help Elliott out of his incubator and hold all of his tubes and wires – Cindy barely moved as she was afraid that she might interfere with them or make him uncomfortable. Overall, Elliott stayed at St. Michaels NICU for 5 weeks before he and Cindy transitioned to a different ward so that they could establish breastfeeding. They soon returned home and, Elliot and Elliott has not required any medical interventions since. Cindy felt that the staff at St. Michaels NICU supported her well, and explained everything that was happening in an easy to understand way. She said: “we felt that our little one was in the best possible hands.”. Talking to other parents at the NICU was one of the things that helped her through, as it made her realise that she was not alone in her situation. Elliott was in an incubator for the first two weeks and Cindy found it very challenging (as I’m sure any parent would) to bond with her baby, especially as most of his care was carried out by the NICU nurses. Slowly, the nurses showed Cindy how to care for Elliott, and talked her through what he needed. Cindy found it quite difficult to organise herself between her time in NICU and while preparing for her son’s arrival at home. Her family lives in France, so being far away from them was not easy for her. Luckily, she had some friends in Bristol that were able to provide her with support. Some advice that Cindy would give to parents in a similar situation would be “Do not hesitate to ask for support from friends and family, and to go for a walk outside of the hospital to get some fresh air, a meal, a coffee... Take some time outside of hospital as well to prepare for your baby's arrival at home, the time will come very soon! Share contacts with other parents to see the roommates of your little one growing at the same time as yours, and share your worries and your good times as well!”.
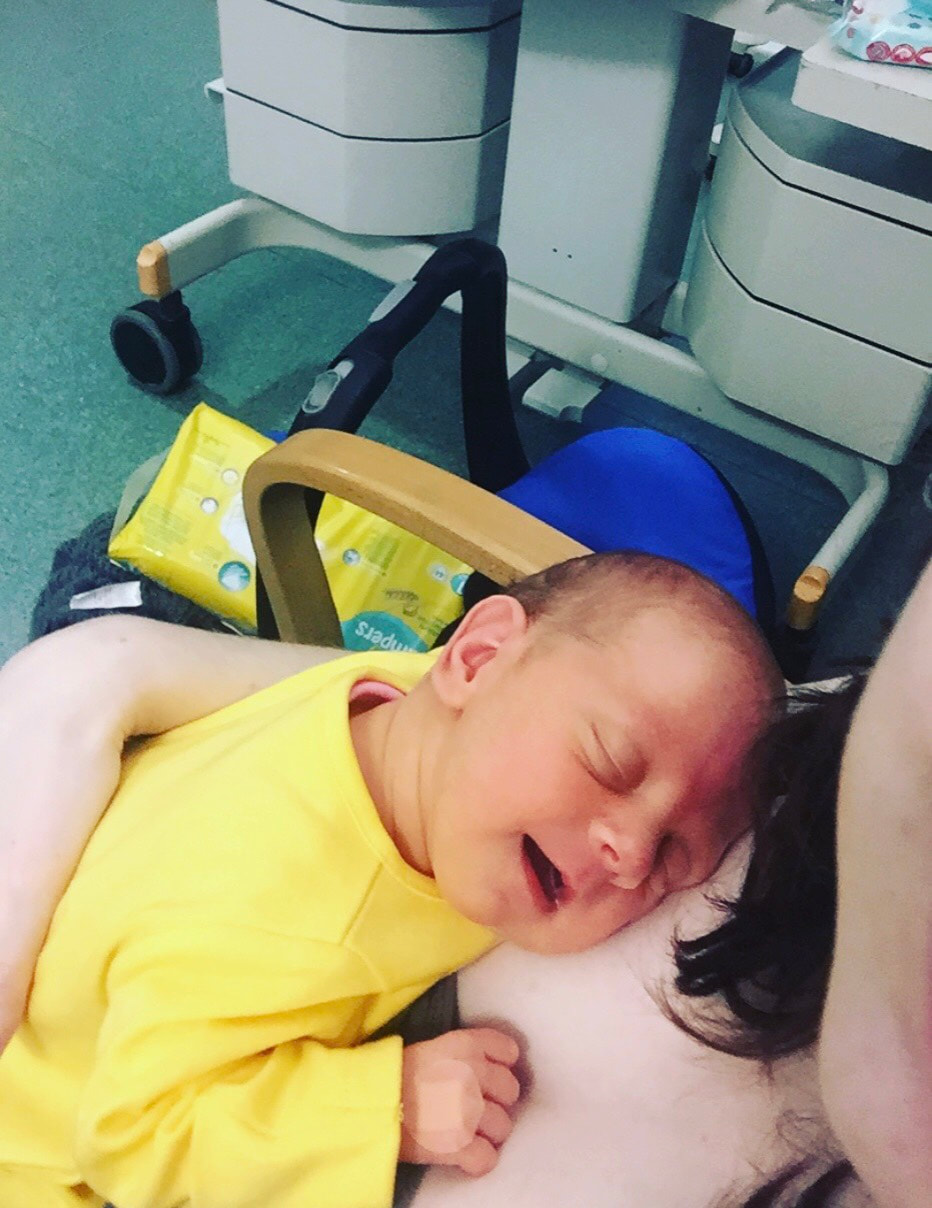
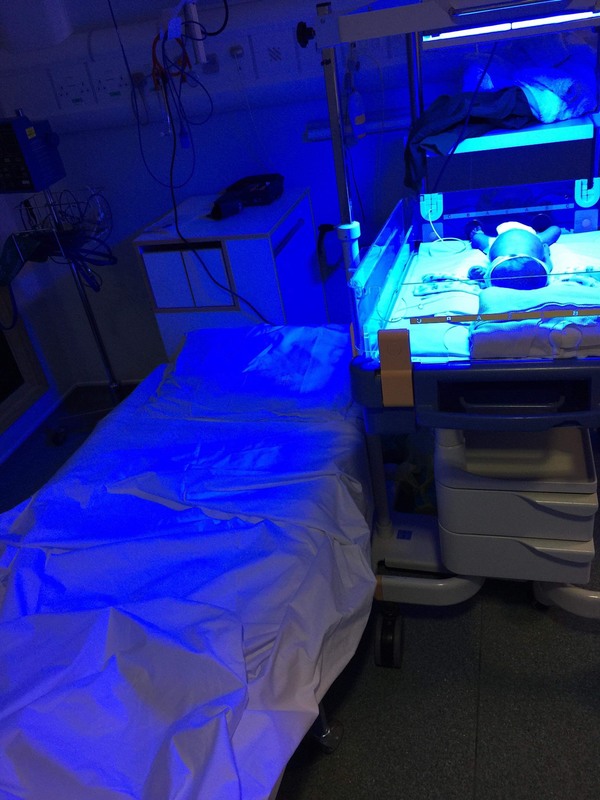
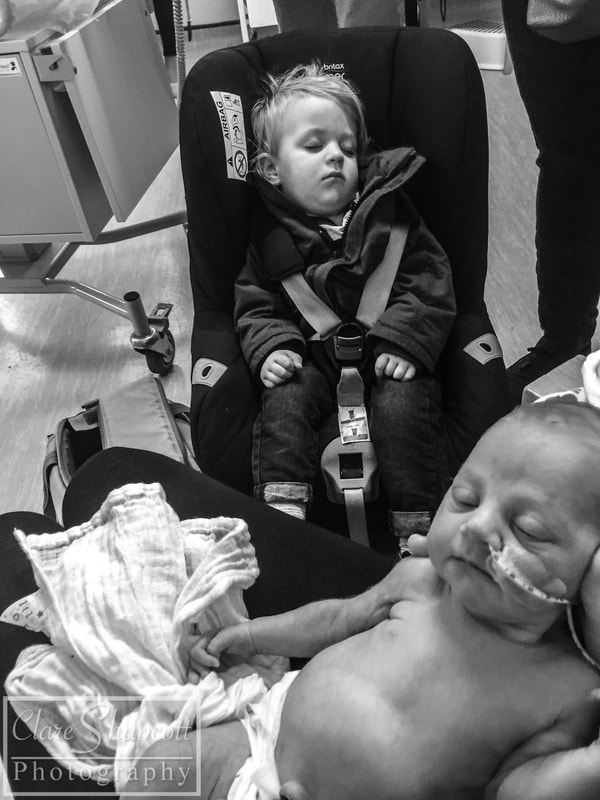
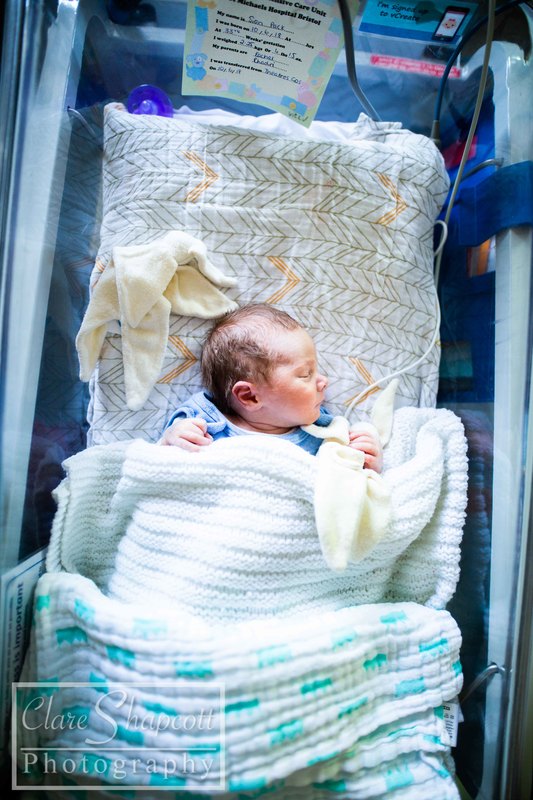
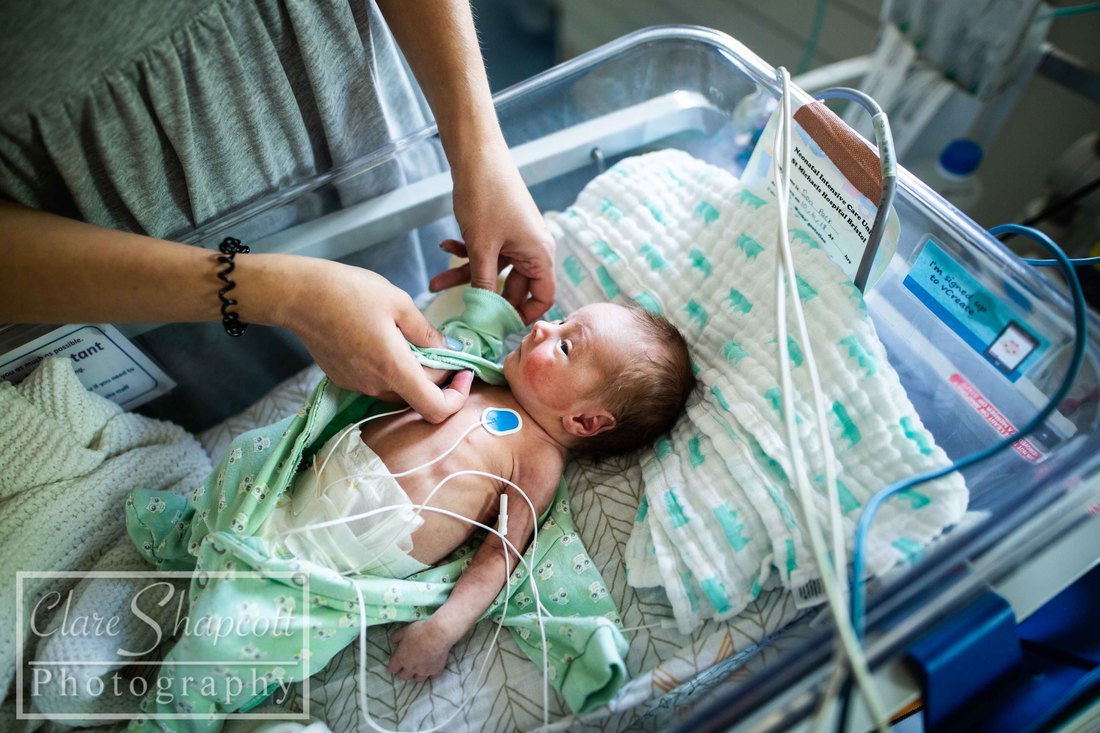
Jess did so well during her first two weeks. She started off as a whopping 5lbs 5oz baby, which sounds tiny but for a 33 weeker, it was good. She spent only 11 days in the NICU and fed and gained weight well. The only thing she couldn't keep on top of was her jaundice. Myself and my husband, Matthew, had a new arch enemy - called Billy-Rueben (elevated Bilirubin levels indicate jaundice). While we were in NICU, Jessica's levels went over treatment levels and she was treated using UV light. This was always gutting as it was a step backward in terms of bringing her home. She was just under treatment level when we were discharged and we were so happy to be going home, we practically forgot all about it. A few days passed and Jess had her normal checkups. She was frequently changing colour and looking yellow for a few hours and then back to normal. It was at one of these checkups that they decided she needed another blood test to check how her levels were doing. We didn't think much of it and carried on with our day. I had a phone call later that day and, unfortunately, we would need to come in and be seen. It was then explained that we would not be able to come back in to Southmead NICU as we had been discharged and Jessica was over 8 days old. We were advised that we should go to the A&E department at the BRI. They would send over the relevant information and Jessica would be given immediate treatment. Unfortunately, they had recieved no records for Jessica on arrival, and so we had to wait to be seen and her treatment was not started. Despite all this, both Jessica and my son, Finley (21 months at the time), were amazing. My husband had to take our son home, despite being anxious to know what was going on with Jessica, which must have been challenging for him. Eventually, a consultant came to see Jessica and advised that she needed to start the treatment ASAP and not wait for all the information to come through. He explained that both premature and breastfed babies had higher risk of developing jaundice and it was completely normal for up to three weeks. Since Jessica was nearly three weeks, he suggested taking some extra blood tests so that they could do further investigations more quickly if she was still struggling past three weeks. It was a few hours until we were moved onto the ward. It was different at the ward at the BRI, compared to Southmead NICU, in that I was solely looking after Jessica. She was under the lights and so this meant that I could not leave the room at all for the entire time I was there. As mentioned in my previous blogs, I was also struggling with lockjaw due to a impacted wisdom tooth. I was completely unable to open my mouth and therefore unable to eat anything, so I had been prescribed fortisip. At the BRI, they provide free meals to all breastfeeding mothers (which is brilliant), however, being unable to eat anything solid, I ran into a problem when I ran out of my fortisip drinks. For about two days, I was only able to consume yoghurt, protein shakes and coffee. Not a brilliant diet for a breastfeeding mother. The second night that I was in the BRI, Jessica was very agitated. As pictured above, the bed was not within reach of her cot. I had to hold her hand and stroke her head to get her to sleep as I could not pick her up to cuddle her. This was due to her being under lights. I was actually very lucky at the BRI, as in the NICU, babies under lights were still in incubators and so it is even more difficult to touch, feed and change them. The third night that she was under lights, I noticed her looking significantly more healthy and the whites of her eyes were no longer yellow. I also was given a pop up bed in the room to allow me to be closer to her and soothe her without having to get up and walk over every few minutes. However, due to a condition I have which makes me extra sensitive to specific UV rays (PMLE), I developed a rash where my skin was exposed to the light. Matthew and Finley came to visit us every day. It was more of a struggle with Finley as he didn't have much to do in the room and as I explained before, we couldn't leave the room with Jessica under the lights. It was the only time that me and Matthew could spend time together as well, as he took Finley home in the evenings and for naps, so we didn't want to split up. Over the course of two days, the doctors and nurses contemplated whether to discharge us. When we were finally discharged, I was so relieved and nervous at the same time. I had felt that I had got my hopes us about keeping Jessica at home the first time and then this had happened. What if it happened again? I'm happy to say this was the last of our hospital visits with Jessica and she is now almost one year old and is happy and healthy!
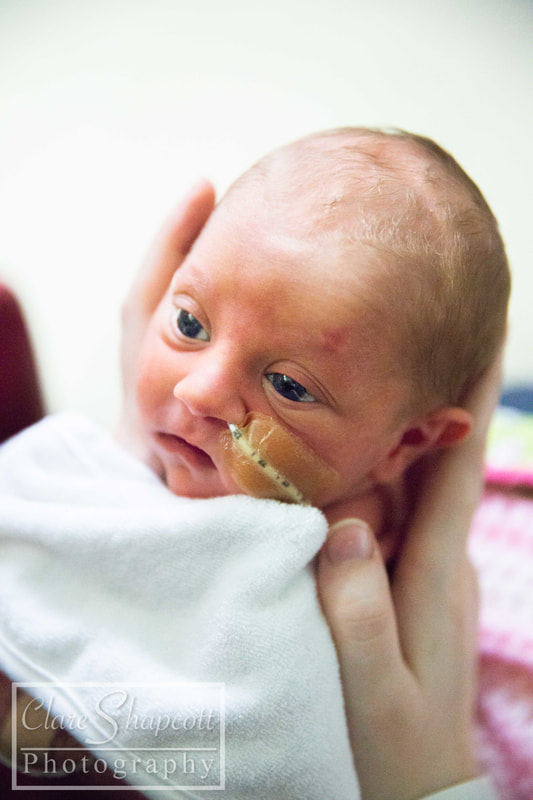
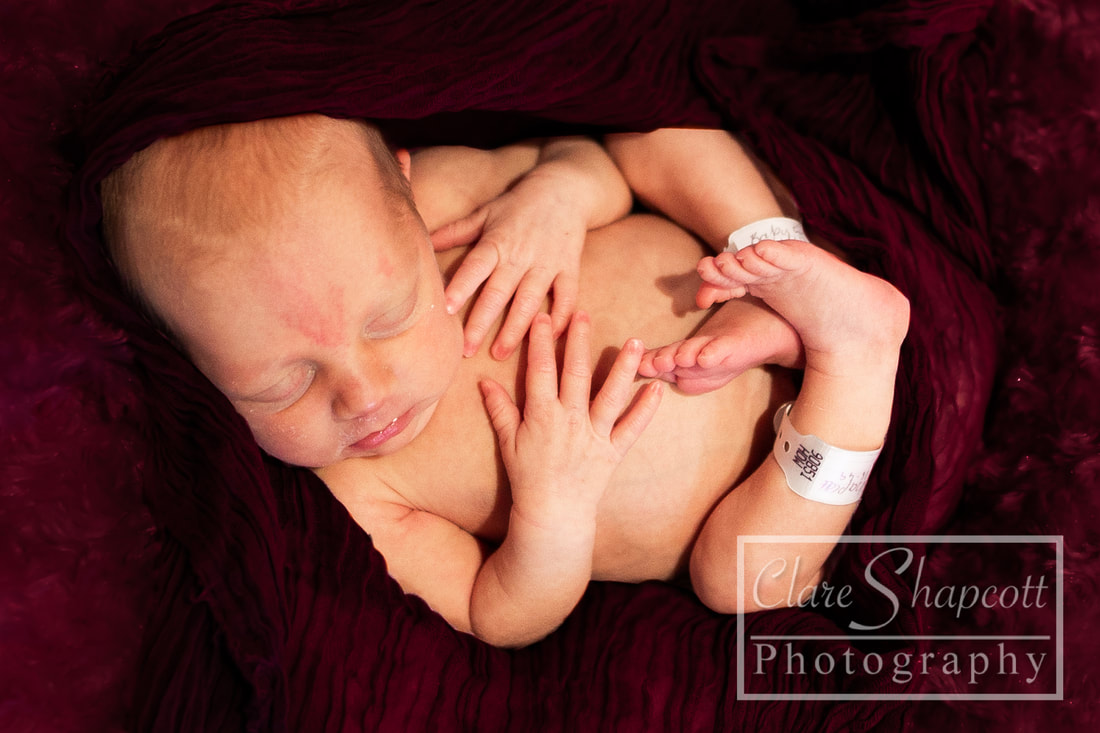
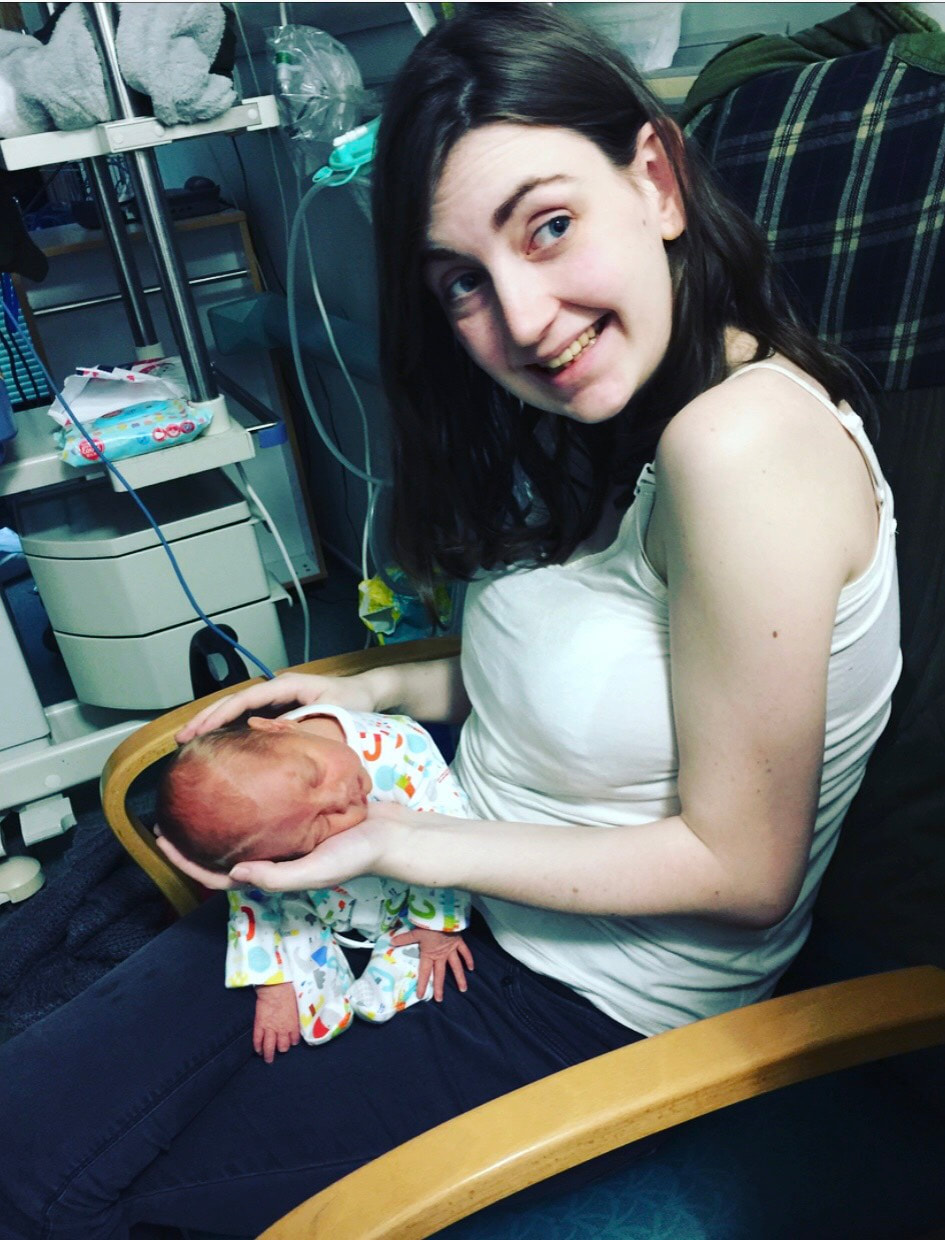
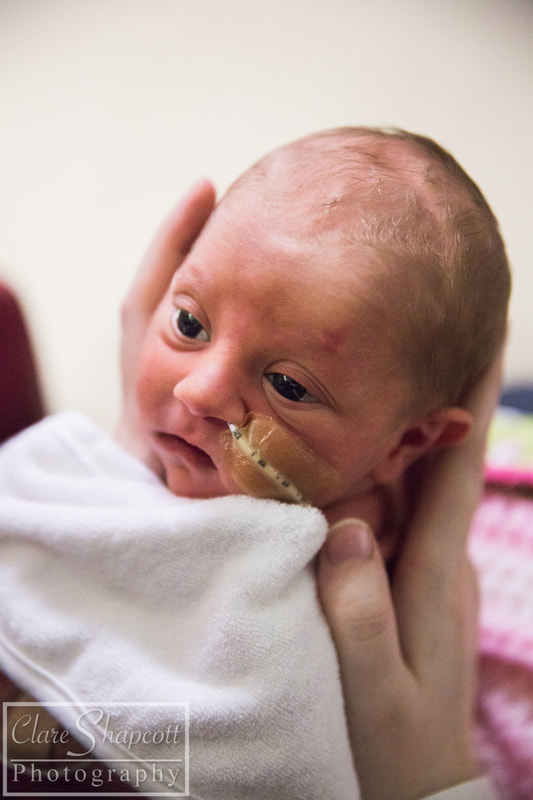
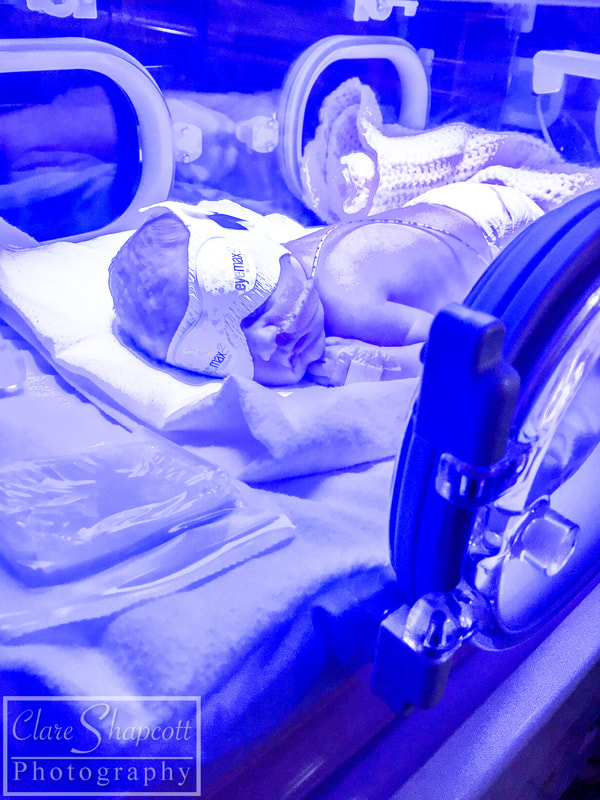
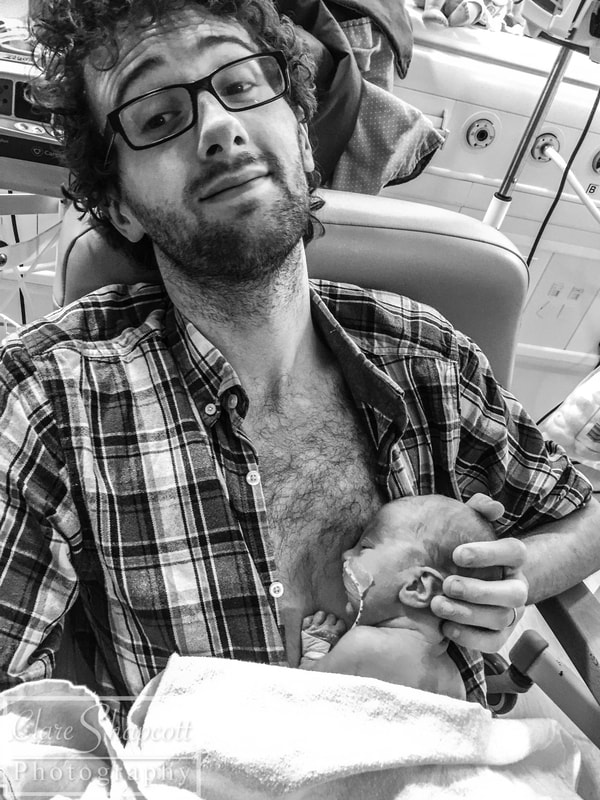
Hello everyone – Clare’s husband here. Clare has asked me if I could write a little blog post for her about her our daughter, Jessica’s, time in NICU, so here it is! After a long, exhausting labour, Jessica was born at 33+6 weeks at Southmead hospital. Her early arrival was completely unexpected, and I felt completely unprepared. During labour, Clare and I were very worried about whether or not Jessica was going to make it. I knew nothing about what it meant to give birth so early, so I had no idea about what complications could arise. After 30 hours of labour, Jessica finally arrived. There were no immediate signs of any health concerns, so she and Clare had a quick cuddle before she was transferred to an open cot and her health was checked by paediatricians. Thankfully, she was in good health, but because she arrived so early, she was taken to the NICU into one of the special care rooms. I walked there with Jessica, beside her in her cot, but Clare was left in the room she gave birth in with her mum, and she felt sad that she couldn’t be with Jessica. I was overwhelmed with emotion, but I just remember being so happy that I had finally met her. After saying goodbye to Jessica, I went home to drop my mother-in-law at home with our son and to pick some things up for my and Clare’s stay at hospital. While I was away, Jessica was moved from the special care room to one of the high dependency rooms. Unfortunately, the midwife who was organising Clare’s arrival to NICU was not informed about Jessica’s room change. So, as you can imagine, when Clare arrived at NICU with the midwife not knowing where our daughter was, there was a bit of a panic! Thankfully, Clare was swiftly reunited with Jessica, and, with my return, our NICU journey had officially begun. Jessica’s stay in NICU was very difficult for us. For three days, we were allowed to stay in one of the hospital wards just a stone’s throw away from NICU. Clare had a hospital bed and I slept next to her in an arm chair. Although it was not the comfiest of places to sleep, I was so exhausted from the previous night’s sleep (or lack thereof) that I had no trouble getting to sleep. Many times throughout the night I would wake up, pop on my shoes and just walk down to the NICU by myself to just look at Jessica through the incubator glass, or (if I was lucky enough) give her a cuddle on my chest as I sat in a reclining armchair. I felt so happy whenever I was with her. She was so small and so delicate. Being at NICU made it difficult for us to spend quality time with our son Finley, who was almost two years old at the time. We had to balance our time so that we were able to care for both our children. Luckily, the NICU at Southmead Hospital had a couple of family rooms filled with books and toys for Finley to read and play with whilst Jessica was in her incubator next to him. Going back and forth between NICU and home multiple times a day was quite exhausting for me. Just the fact that Jessica was in NICU in the first place was emotionally overwhelming. I felt so emotional one evening whilst driving back to NICU. I was listening to a song called “Waitin’ for a Superman” by The Flaming Lips as I was driving to NICU on my car stereo, and it just made me think about how incredibly challenging it was to be a NICU parent. I thought about how everyone was counting on me to be strong and resilient, but it was just too full on for me to manage. When the chorus arrived, I just started to cry while I was driving. After three nights, our night time stays at Southmead Hospital had come to an end. The NICU ward had some spare rooms for parents who lived far from the hospital or for families who’s baby were almost ready to be discharged. We didn’t fit into either of those categories, but I strongly felt that it was important for Clare and Jessica to stay close to each other. With Clare knowing that she wasn’t going to be saying on the ward anymore, she had stubbornly decided that she was going to just sleep on the armchair next to Jessica’s cot, in the same room as all the other newborn NICU babies. I admire her willingness to be there for Jessica – it was important for Clare to be nearby if she and Jessica were going to develop a good breastfeeding regime. I didn’t, however, think that it was a good idea for Clare to sleep on an armchair for the next however many days, so I decided that something must be done. I was able to persuade one of the head midwives to allow Clare to stay in one of the spare rooms, under the condition that if someone else needed a room, she would have to be evicted on short notice. That was incredible news for us, as it meant that Clare could be closer to Jessica, and, in a few days time, it would happen that Jessica was allowed to sleep in the same room as Clare. Unfortunately, there soon did come a day when someone needed the spare room more than Clare. Clare had to leave, and she decided that it would be best if she did come home instead of sleeping in the armchair. She was still very determined to breastfeed Jessica as much as she could, so she timed her NICU departure and re-arrival at such times so that she would only miss two feeds. Although she had been able to come back home every evening since she was discharged to have a bath with Finley, she was able to spend some extra time with him, and she was even able to have a short, but comfy sleep in her own bed. Luckily, she was given a room again when she returned! Although I was allowed to stay with Clare and Jess, we decided that it would be best if I returned home to stay with Finley. I was sad to be leaving Clare and Jessica at hospital, but I was also happy to be able to spend some nights at home with Finley as well. I felt a bit inadequate, in the sense that I wasn’t there to give Jessica cuddles, or change her nappy, or comfort her if she was crying. I trusted Clare and the NICU midwives to be there for Jess, but I still wanted to be doing more for her. During Jessica’s stay at NICU, there was a constant battle between whether or not she required treatment for jaundice. She was quite yellow, and during the first few days of her life, her bilirubin levels were quite high. She needed to be put under ultraviolet lights to treat her Jaundice, for which she needed to wear special eye covers to protect her eyes. After a few days, her bilirubin levels lowered, and the UV lights weren’t needed. Unfortunately, her bilirubin levels kept increasing to just over the threshold for her requiring UV light treatment and she kept on being put under lights. It was great when I arrived at NICU and saw that Jessica’s general health had improved. After saying goodbye to her in the evenings with the UV lights above her, seeing her in the morning with the lights removed and in an open cot would put a smile on my face. Another big thing was when her nasal cannula and feeding tube (which entered through her nose) were removed, and we could see her face a bit more clearly. As Jessica’s health improved, she was moved to different rooms which required less intensive care. Some mornings I would walk in and not realise that she had changed rooms, so it was a nice surprise to see when her room had changed! On her last day, Jessica had shown to be feeding well, and her bilirubin levels had settled to an amount that didn’t require treatment. This meant that the midwives and doctors could discharge her from NICU and we could take her home! Clare and I were very excited and so relieved to be finally taking her home where it would feel a bit more like we were a family. We are so incredibly grateful for the care and medical expertise that the midwives and doctors provided for Jessica during her stay. We are also thankful for Clare’s mum, who flew to Bristol from France to support us all and take care of Finley while Clare and I were at hospital. Our friend Maddie was also kind enough to make us some delicious meals which really helped, and also Helen was very helpful when she looked after our son Finley, so a big thank you to them, as well as everyone else who helped out! If I were to give some advice to other dads with babies in NICU, I would say don’t be afraid to ask for help and support from friends, or to ask any questions to the midwives and doctors. People may not know what it is like to be in your position, but they do understand that it is a difficult and stressful time for you, and I am sure they will be happy to help. If you would like to read more about Clare's Pregnancy and birth, please see previous blog posts:
Rainbow Pregnancy Project Part 1 Rainbow Pregnancy Project Part 2 Jessica's Surpise Debut Jessica is currently a thriving (nearly) one year old, however unfortunately her NICU story was not the end of her early hospital stays. Clare will be writing about her struggle with jaundice soon, so keep an eye out for her next blog post! I met this incredible mum, Paige, and her 6-month-old son, Marleigh, at St. Michaels hospital a few weeks ago. Their journey from early pregnancy to where they are now has been truly awe-inspiring, and they have both been very resilient. Paige’s pregnancy began as normal as any pregnancy should be. She was feeling nauseous, she had morning sickness, and she was completely put off certain foods. Her 12-week and 20-week scans were normal, and she was happy to find out that she was expecting a boy! Soon afterwards, her hands and feet started swelling up, and she soon developed carpel tunnel syndrome. After her doctor found that she had high blood pressure, she was admitted to hospital, and put on high doses of blood pressure medication – she ended up having to take more than 20 pills per day! Apart from her high blood pressure, Paige felt fine. She was starting to wonder why she was even being kept at hospital. However, at 25 weeks the doctors noticed that Marleigh had stopped growing. Paige’s placenta was no longer sending Marleigh food, but it was still supplying him with oxygen. Because of this, the doctors decided to keep him in there to mature. At 26+4 weeks, Paige developed severe gastric pain which spread to her back. She was given medication to treat heart-burn, but Paige knew that the problem was more severe than that. Her pain was unbearable, even when taking various painkillers including morphine. The next day, after having only slept for 2 hours, she was rushed to Derriford hospital in Plymouth, which is a hospital that can more easily handle pregnancies at young gestations. A scan later showed that Marleigh was stable, but unfortunately Paige’s platelet count was extremely low, and the doctors diagnosed Paige with having HELLP syndrome. Twenty minutes later, she was rushed into the high dependency room for an emergency c-section. Doctors and nurses flooded the room to ensure that Paige and Marleigh were both cared for. The doctors gave Paige multiple cannulas where she was given magnesium and blood pressure medication. At this point, her blood pressure was 240/98 and it needed to go down to 160/100 before she could enter theatre. Paige was feeling so frightened at this point, but soon, fortunately enough, Marleigh arrived safely, and was taken to NICU. Marleigh was diagnosed with having Pierre Robin sequence, which caused him to have an abnormal airway. Because of this, for fourteen hours, he required a makeshift breathing mask, as he was not able to tolerate CPAP. Paige felt very grateful for the nurses there. Paige and Marleigh were transferred to their local hospital in Truro, where they stayed for 2 weeks before needing to be transferred to St. Michaels hospital where Marleigh has been given a bit of extra support. Paige and Marleigh have been a super Mum and Son duo and have been so amazing to deal with all the difficult issues facing their health. Paige says that one of the most difficult things that she has to deal with is having to make big decisions about Marleigh’s health. She also says that she feels heartbroken whenever the emergency alarm goes off for Marleigh and the doctors and nurses rush around him. One thing that makes Paige feel happy is seeing him smile and play, and watch his health improve day by day. She is very thankful for the support that she has been given by the nurses at NICU, but also from her mum and her partner. Some advice that she would give to other mums in a similar situation is: “Try to keep as calm as you can and also make sure you get some rest.“
I've decided to write a blog post today about crafts for various aged children for halloween. I've also included links to many more craft idea's that we're yet to try! If you are looking for something to do for halloween this Saturday 27th, please join me at Doddington Parish Hall to help raise money for Southmead NICU. I will be offering halloween photoshoots, suitable for all ages, and donating 20% to Southmead NICU. More details can be found at the bottom of this blog post. Pumpkin stamps1) Cut an apple in half 2) Paint the flat surface orange and the stalk green 3) Stamp on paper 4) Draw on pumpkin face For more detailed steps, see here: http://www.frugalmomeh.com/2015/09/pumpkin-apple-stamps.html Mason jar Mummys1) Find any clear jar and remove lid 2) Wrap masking tape around jar 3) Draw across the lines and add goggly eyes 4) *Adult help for this step* Light the tea-light in the jar For more lantern ideas, have a look here: https://rhythmsofplay.com/top-10-diy-halloween-lanterns/ Ghost Footprints1) Using baby friendly paint and a sponge, apply paint to baby's foot 2) press foot firmly on paper 3) Complete design with paint or pen when dry For more hand and footprint ideas, see here: https://www.craftymorning.com/adorable-handprint-footprint-halloween-crafts/ Mummy monsters1) Draw mummy's eyes on cardboard tube 2) Ask toddler to wrap masking tape around the roll and eyes! Many more halloween craft ideas can be found here:
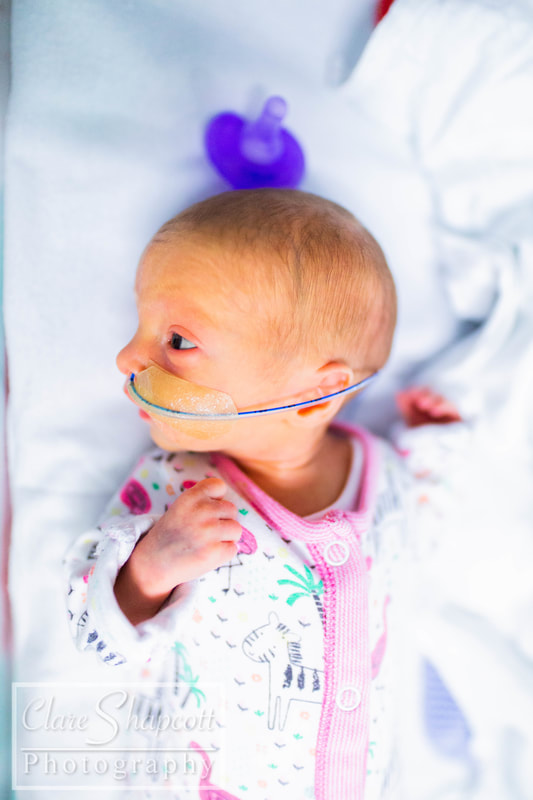
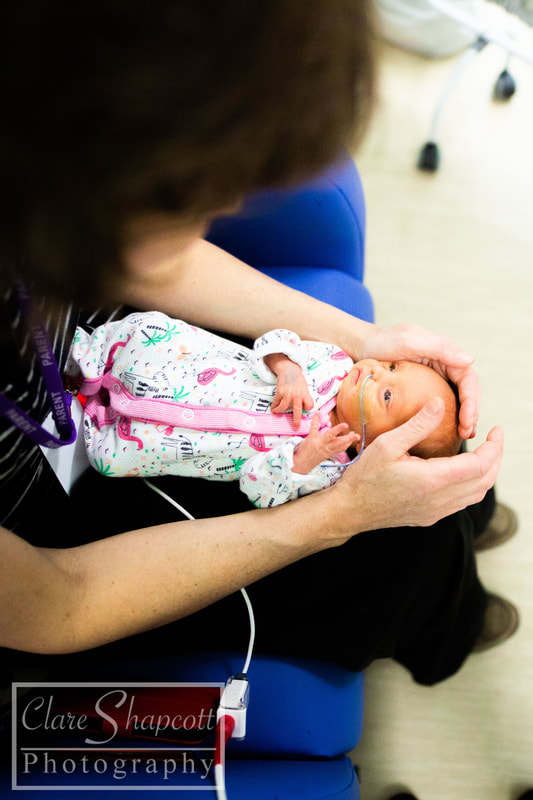
https://farmfoodfamily.com/diy-halloween-crafts-for-kids/ I recently went to the NICU at St Michaels Hospital to meet and photograph a lovely mother, Rachel and her little warrior son, Sion. Rachel's pregnancy started free of complications, which she was grateful for. Sion was monitored for growth after Rachel's partner, Rhodri, tested positive for the Zika virus - a virus passed on by mosquitoes in some parts of the world. He caught it when he was working to support the hurricane relief in the Caribbean as a corporal in the marines. Sion's growth seemed to be doing well, so there wasn't much to worry about. At 32 weeks, the family had a scare when Rachel came home from work early, feeling very unwell. When she called in, she was advised to come into the hospital. She felt that this was over the top and unnecessary, but came in anyway. She was told that her temperature was high but there were no major complications. Sion's heart-rate dropped and continued to do so, so Rachel was put on a drip, which she hated. She continued to feel unwell and eventually was sick. Rhodri just about managed to get the bowl to her in time! They were told that if Sion's heart-rate dropped once more, they would have a C-Section that night. Rachel had never felt more anxious in her life. Fortunately, Sion's heart-rate remained the same throughout that night. The next day was much less eventful. By evening, Rachel was finally allowed to eat again and Rhodri bought her nandos which were, in her words, 'the best thing ever'! Rachel had to have an amniocentesis to ensure the infection hadn't spread to the womb. She had to see the needle next to her baby in the scan. It was terrifying. Luckily, it came back negative, For four days, Rachel continued to be monitored. Rhodri was told to come and pick Rachel up under the assumption she would be discharged. Instead, Sion's head had engaged and they were told he would be coming! Rachel said she'd 'never forget the look on his face'. She was then induced, and describes using the 'daisy breathing' technique to help her with the pain. She found her waters breaking very uncomfortable. Shortly afterwards, Sion's heart-rate dropped again. They decided to have a C-Section. The experience was, as Rachel described, 'bizzarre'. Her arms were shaking very fast. Suddenly, Sion was there and he cried. Sion was born at 33+4 weeks and he weighed 4lbs 15oz. Rachel was allowed a quick cuddle and then he was taken to an incubator. She didn't get to have skin to skin, which made her feel disappointed. Alongside the irreplaceable support of Rhodri, her mum had been with her during labour, which had been amazing as she 'felt she could be more vulnerable with [her] mum'. Sion needed steroids and help breathing at birth. He also had 3 lumber punctures, caffeine and lots of antibiotics. He was very poorly with sepsis and viral meningitis. Sion was in NICU for the first three and a half weeks before they moved to the transitional ward for 3 days. Rachel hated the transitional ward and just wanted, understandably, to take her baby home! The biggest challenged Rachel had was the separation at birth. She missed her 'bump' and having her baby close to her. Seeing Sion poorly was disheartening and being discharged without him was completely heartbreaking for Rachel. She cried all night, but woke up excited at the thought of seeing him again. Even weeks later, Rachel still hates the thought of it. One of the happiest moments for Rachel was when Sion came off CPAP, as she could finally see his face and his hair properly. The day he was rid of all his wires made Rachel so happy. Of course, bringing Sion home, made Rachel feel even happier. In the hospital, the staff, both at the delivery suit and in NICU, were amazing. Rachel's nurses were incredible with Sion and she will always be grateful to them. Rhodri, Rachel's mum, sister, family and friends, as well as Rhodri’s family were her rocks. Since being home, they have been so supportive, she feels she couldn't have done it without them. Rachel wanted to add a few words:
"Ask so many questions and don’t worry if you’re being an overbearing and over anxious Mum! They are the experts and before you know it you’ll be home and on your own and that is very daunting when they’re so small. Get as much help as you can whilst they’re in there to help prepare when you go home! I am so grateful to my partner family friends and the staff at St. Michael’s for looking after me and my baby. We are very lucky to have had such great care and continue to have such great care from the people around us. Thank you Clare for the beautiful photographs. It’s a lovely thing you do for poorly babies and their families! Thank you xxx" I recently met with a mum, Sarah and grandma, Margaret of a lovely boy who started off his journey, like my Jessica, a little bit earlier than expected. After their experience, they felt compelled to raise money to help support Southmead NICU in any way they could. They currently run Little Tiddlers Market events, which brings small businesses and families together for afternoons of fun! Today, I'm going to tell you a bit about their time in NICU, a review of their market as both a mother and a small business owner and some information at the end on event dates, deals, and how you can help.
The market itself is held at Iron Acton Parish hall. It consists of a variety of different stalls, including Usborne Books, Younique, Linelife, Bouncy Castles, Partylite, Forever Living, Avon and of course, Clare Shapcott Photography. Each event also tends to have an array of independent creative businesses. I have seen handmade cards, florists, handmade jewelry and a variety of beautiful crafts. There is always a happy vibe between stall holders, and Sarah helps to make sure of this by only booking one of each type of stall so that there is no competition. This has the added benefit of giving an amazing variety of products to choose from! On entering the market there is an entry fee of only £1. There is also a chance to play games such as Lucky Dip, Hook a Bag, Name The Teddy, Guess the Sweets, Guess the Hamper and Tombola. All of these games' profits are donated to Southmead NICU. The Toy Stall and the Clothes Stall also donate to the unit. Clare Shapcott Photography runs a variety of photoshoots and vouchers which donate to the unit too. We have been to a few of these markets now and I have to say it's the most fun I have had while raising money to support a cause which is so close to our family. My toddler has a lot of fun looking at the stalls, playing in the play area, eating cake from the cafe and bouncing on the bouncy castle - even making friends while he's there! My baby girl also gets treated to cake... in that I eat a lot of cake and then breastfeed her! Those of you who know my husband will know that he is very frugal and only goes for the best of deals, and even he has come away with clothes and items from the market. As a business owner I have been treated amazingly by Sarah, Margaret and the whole team! They helped me with small tasks on the day, such as lending me a tub to collect donation money and helping me create a big enough sign. Sarah always puts a great deal of thought into the arrangement of the market and has always planned carefully on where to put the stalls to help reach people who are most interested in my services. As a mum, they have been amazing with me. They have supported me to be able to work while having a small, breastfeeding baby. I have felt comfortable breastfeeding there and have been offered a room if I wanted to go somewhere private. As well as having a stall, I also do mini-photoshoots at many of the little tiddlers market events. These are very reduced and some, often all, of the proceeds are donated to Southmead NICU (Please see each event for more info). I have to say, I think the work that Sarah and Margaret put into these markets is truly inspiring. And there is good reason for it. Sadly, the neonatal units don't get anywhere close to the amount of funding they need through the government. The hospitals provide life saving care for babies that otherwise would not make it. The staff at Southmead are incredible and the work they do there is amazing. As always, I have to mention my baby girl Jess, who wouldn't be here today without the amazing care at Southmead NICU. There are a few ways that you can help: 1) Attending the events..Iron Action Parish Hall High St, Bristol BS37 9UH 2pm-5pm
Dodington Parish Hall Finch Rd, Chipping Sodbury, Bristol BS37 6JZ 2pm-5pm
*Clare Shapcott Photography will have a stall at this event (one off deals and vouchers will be offered) ***Clare Shapcott Photography will be offering mini Photoshoots at this event (donations are always made to Southmead Neonatal Unit) 2) Offering Donation of Clothes and Toys...Please contact Sarah on sarahryan2012@hotmail.co.uk to donate any clothes and toys to be sold at these events. 3) Donating Through 'Go Fund Me'...Please do not hesitate to donate here. No donation is too small. www.gofundme.com/raising-money-for-southmead-nicu 4) Taking Part in Competitions and AuctionsSarah runs an online facebook group, which promotes various competitions and auctions and has more information about the events being held and the suppliers involved. www.facebook.com/groups/147499866025244
Shortly after bringing Jess home, I decided it was time for some family photographs. We often go to the woods near our house for a little walk and I always think of how beautiful it would be to take photographs there. Being nearly two years old, Finley got distracted by many things on the way there and ended up wanting to be carried by daddy, who was already carrying my camera bag and tripod! Jessica slept most of the way there, but since mummy couldn't quite make it over the stye with her in the sling, I ended up passing her over to daddy. She didn't sleep through the transition but remained calm. We walked around the woods as usual and Finley enjoyed looking out for the wooden animals which were dotted around various points around the forest. We settled in a spot and I began to set up. As you can probably imagine, Finley did not want to stay put. I set up the tripod behind a low hanging brach to add in some leaves in the foreground of the image. I then manually focussed on the logs I wanted us to sit on and did some test shots. The family (as pictured above) did not take these shots too seriously! I set the camera on a timer and we attempted to lure our toddler over to where we were. This went as well as could be expected. Finding creative ways to entertain toddlers is one of my husband's many talents. He ran around with Finley for the seconds before the shot and quickly sat down and asked Finley where the camera was at the last second. Finley actually wanted to sit on my lap so this one wasn't too difficult. You may notice his foot is sticking out slightly towards the log next to us. This is because between every shot Finley would kick the log down and laugh when daddy kept rushing to put it back up and get out of the way as quickly as possible. Jessica and I were ready for a nice mummy and daughter photograph, when the boys photobombed us. Finley thought Jessica's yawning was hilarious. Of course, while we were there, I decided to get some couple photographs of us in. This doesn't happen very often! Partly because we are always looking after the kids and also because my husband is not very good at doing what he's told and I get easily frustrated. He did okay this time though. All in all I'm glad we did it as it's such a precious time to capture these moments as a family, even if it was a bit frantic!
I recently visited a mother and daughter in my local neonatal unit. For various reasons they would prefer not to be named. To avoid confusion, I will refer to the mother as Beth and the baby as Lucy throughout this blog post. Beth found her pregnancy quite intense. She suffers from lupus and was increasingly symptomatic during her second trimester. At 28 weeks, it became apparent that Lucy's growth was trailing off and complications seemed more likely. There was a chance that they would need to deliver the baby imminently, however their obstetrician aimed to get them to at least 32 weeks. Amazingly, Beth made it to 34 weeks before having a cesarean section. The moment Lucy emerged during the procedure was one of Beth's happiest moments. During the chaos of it all, it is so important for all NICU parents (and parents in general) to take in these beautiful moments and keep them with you. When Lucy arrived, she was taken straight to NICU for monitoring. Apart from being very tiny, she did not need much medical intervention at all. Beth describes the moment when she first held Lucy against her skin as a very special moment. Beth was discharged after only four days but was lucky enough to receive accommodation nearby. This was something she was extremely grateful for as it made it possible for her to spend more time with her baby girl. Within the first week, however, Beth was suspected to have a bug. As a result of this, she was kept away from her daughter for 42 hours. This was the most difficult part of Lucy's stay in hospital and was heart breaking for her. Babies who are sick or premature in the NICU are so much more susceptible to illness. It is completely heartbreaking to not be able to hold or be with your baby. Knowing how necessary it is and how it is in the best interest of your baby, does not take away the pain. Grandparents and other family members are generally not allowed to have physical contact with the babies at all. Beth and Lucy had an amazing support network with friends coming to visit, being supplied with meals and help with transportation to and from hospital. She also enjoyed conversing with other parents in the NICU and advises anyone in a similar situation to "Talk to other NICU parents; they are a great source of information and support and there is a strong sense of community. I met so many other parents who inspired me with their courage and determination." Beth describes the staff that cared for Lucy as 'brilliant', and they made a great effort to include her partner and herself in their daughter's care. Other benefits the hospital offers to NICU parents, such as free parking, meal vouchers and access to the staff cafe can make a huge difference. Lucy spent three and a half weeks in the NICU, primarily to make sure she was putting on enough weight. Taking her home from the hospital was another amazingly happy moment for Beth.
|
Clare ShapcottPhotographer Archives
December 2021
Categories
All
|






















































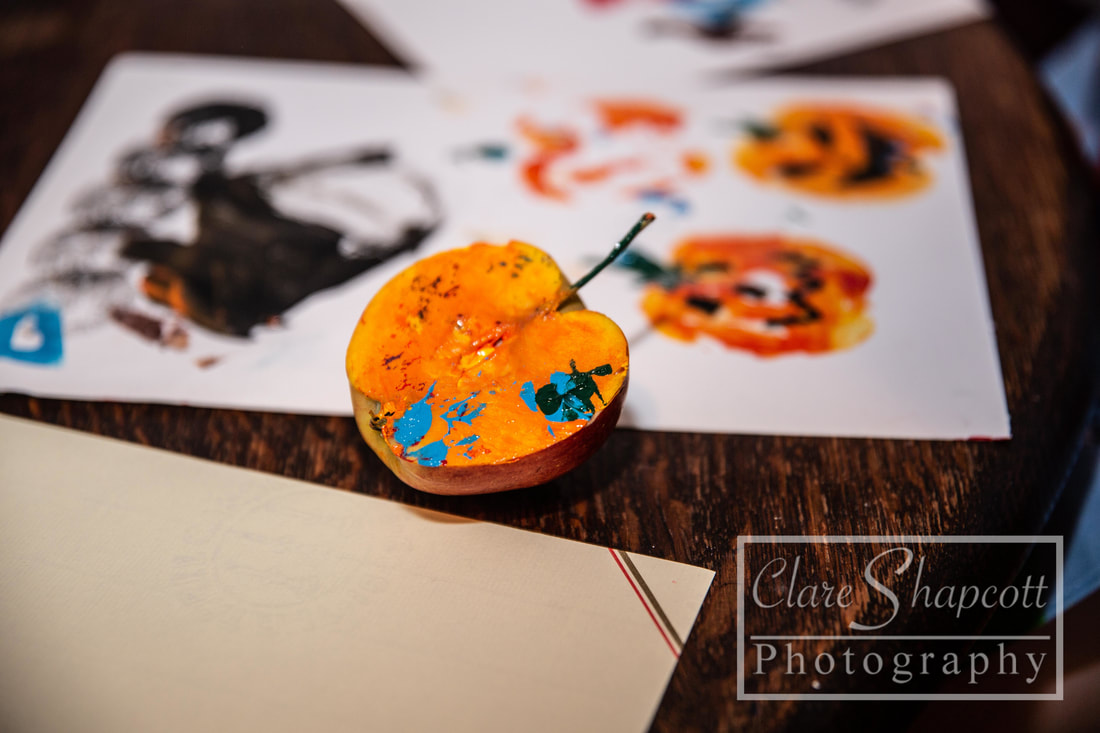









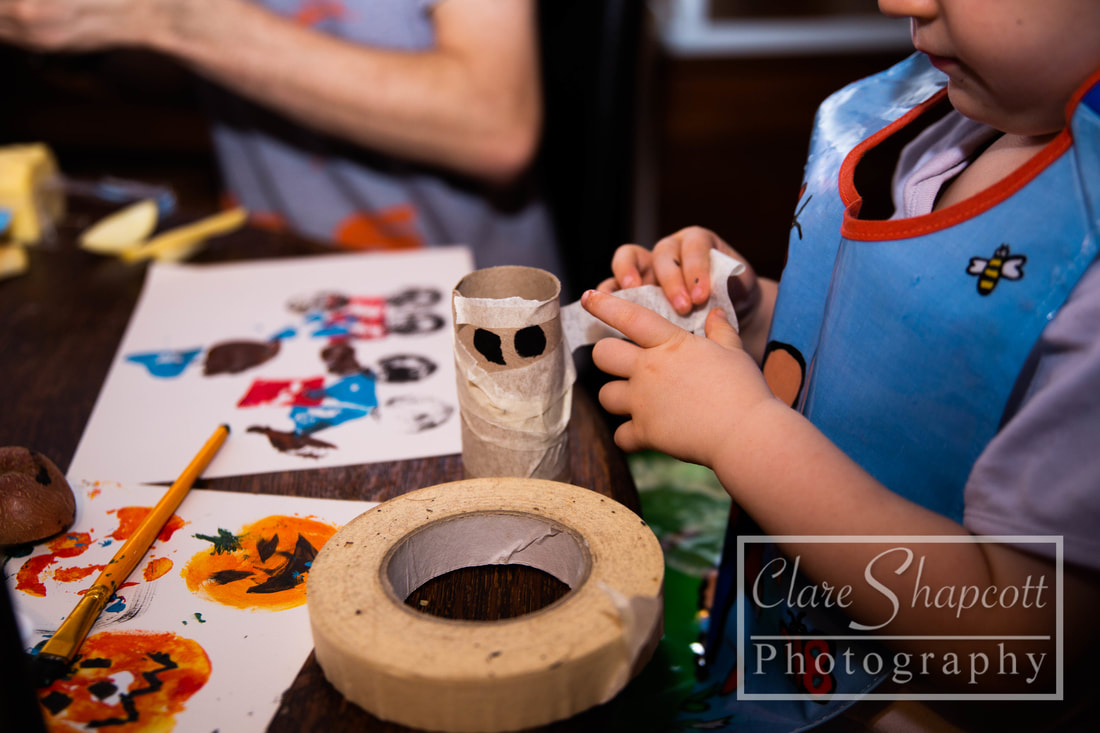










































 RSS Feed
RSS Feed







